- Privacy Policy
- Terms & Conditions
- Contact us
- ©Isabel Healthcare 2025
1 Minute Read - Tickborne Diseases - The Great Imitator
 Tickborne diseases are infectious pathogens transmitted by tick bites to humans.
Tickborne diseases are infectious pathogens transmitted by tick bites to humans.
In the United States, the most common tickborne diseases are:
- Lyme disease
- Babesiosis
- Ehrlichiosis
- Rocky Mountain spotted fever
- Anaplasmosis
- Tickborne relapsing fever
- Tularemia
Within the UK, the most common tickborne disease is Lyme disease.
How do tickborne diseases occur in humans?
Ticks are great vectors for disease transmission and are the second most common vector after mosquitoes. There are more than 800 different species of ticks living in the world. They transmit disease by waiting in low vegetation, finding a suitable host in the form of a mammal, reptile or bird, then attaching themselves to the host to feed. They do this by inserting their hypostome (feeding tube) into the host’s skin and feeding off the host’s blood. Some ticks also secrete anticoagulant, immunosuppressive and anti-inflammatory substances which prevents the host from noticing the tick has attached itself and is feeding from its blood. These substances also allow the pathogen on the tick’s hypostome to easily gain entry to the host’s body and for the body not to initiate a reaction to combat the pathogen at the time of the tick bite, so the pathogen can establish itself. Pathogens which can be transmitted by ticks include bacteria, viruses, parasites, toxins, nematodes and spirochetes.
Avoiding delayed or misdiagnosis with tickborne diseases
There are quite a few reasons why tickborne diseases are often misdiagnosed or diagnosed late. Here are some of the most common reasons to look out for when assessing a patient’s symptoms:
- As the pathogens invade the host’s body, often without the host even noticing the initial bite, they can lay dormant for a while before the person develops symptoms. Due to this, a tickborne disease is often misdiagnosed as something else, because the history of the tick bite is not known at the point of diagnosis and therefore not linked to the presenting symptoms. A travel history of up to 10 years should be taken.
- Tickborne diseases closely resemble other illnesses which leads to tunnel vision and confirmation bias. Not considering a wide differential can lead to misdiagnosis and delayed or incorrect treatment for patients.
- One tick bite can transmit multiple pathogens, which can lead to atypical presentations of tickborne diseases that don’t fit into the common textbook symptoms of a tickborne disease. Generating a differential using the Isabel DDx Generator will help you consider atypical and typical disease presentations for your patient.
- Many tests for tickborne diseases are negative at the time the patient first presents to their doctor. For example, Lyme disease blood tests rely on a person’s immune response once they have been infected with the bacteria. It can take between 10-30 days for the body to return a measurable immune response and detect Lyme antibodies in the blood. If someone is tested for Lyme before the antibodies are produced, then the result may be a false negative. The diagnosis may be missed due to this and no treatment can lead to more serious complications.
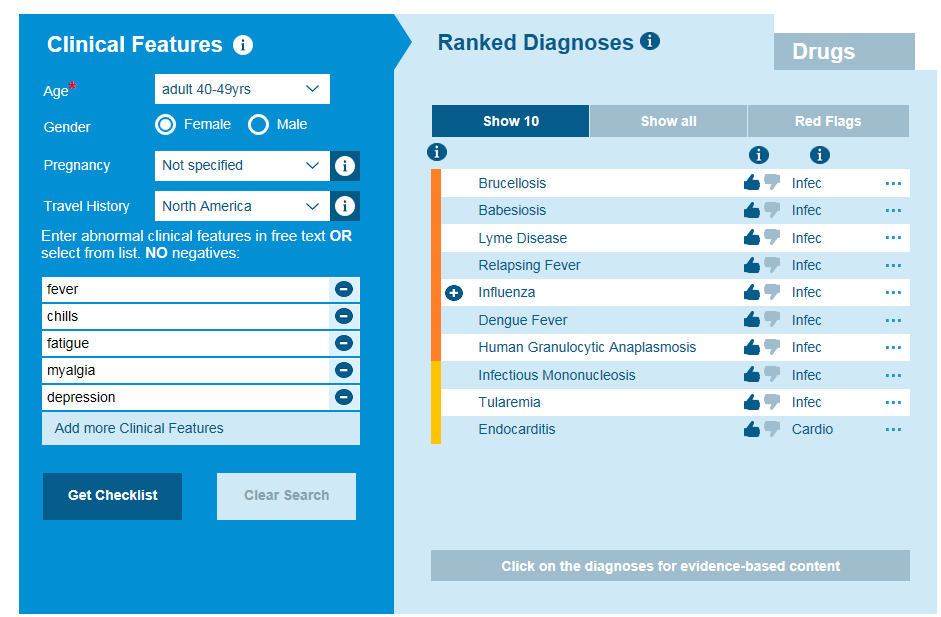
Infectious conditions including tickborne diseases
Common symptoms of tickborne diseases
The symptoms of tickborne diseases are very easily mistaken for other, more common illnesses with similar presentations. Tickborne diseases should be considered with any of the following symptoms.
Flu-like symptoms
The most common symptoms of a tickborne disease are fever, chills, headache, fatigue and myalgia. These common symptoms can be representative of many other diseases including influenza. If a patient presents with these symptoms, then a travel history should always be obtained, and enquiries made as to whether the patient has had a tick bite. Enquire whether the patient has noticed a rash around the bite site or elsewhere on their body. Lyme disease, Rocky Mountain spotted fever, ehrlichiosis, bartonellosis and tularemia commonly have a rash associated with them. In Lyme disease, a bull’s eye rash (erythema migrans) is characteristic of the condition.
Malaria-like symptoms
Babesiosis is a parasitic infection and is the second most common tickborne disease in North America. The most common signs of babesiosis are like malaria and include a high fever, sweating, nausea, headaches and fatigue.
Cognitive symptoms
These symptoms can include confusion, disorientation, memory loss and depression. For example, Rocky Mountain spotted fever can present with confusion, and patients with undiagnosed chronic Lyme disease can experience depression.
Lyme disease - The ‘great imitator’
Lyme disease has a wide range of symptoms, as it can affect many systems within the body, and so it mimics a wide range of other illnesses. These include amyotrophic lateral sclerosis, Alzheimer’s disease, chronic fatigue syndrome, fibromyalgia, and Multiple Sclerosis (MS). Patients presenting with arthritis symptoms including myalgia, chills, headache, lymphadenopathy, or joint pain should also ensure Lyme disease is considered before making a diagnosis of Rheumatoid arthritis. For a patient who has a chronic history and has symptoms of any of these diseases, Lyme disease should be on the differential list, and the patient should be asked whether they recall a tick bite, or if they have lived or travelled in a Lyme disease prevalent area within the last 10 years.
An increasing problem
The number of Lyme disease cases in the UK, and of all tickborne diseases in the US, are on the rise. What’s more, these figures do not account for the misdiagnosed cases or the cases where the diagnosis hasn’t been confirmed. The geographic range of the tick vectors is also expanding as they are found in new areas. Tickborne diseases are challenging to accurately diagnose and present, as they have vague symptoms which mimic many other diseases. A high degree of clinical suspicion is needed to make the diagnosis, especially in the absence of a tick bite history. Raising awareness of tickborne diseases is needed, both among health professionals and also patients, to ensure an accurate and timely diagnosis is made.
Questions to ask patients when considering tickborne diseases
- Where have you been over the last few weeks?
- Have you been hiking, camping or spending time in the back yard?
- Have you noticed any ticks on your body?
- Have you noticed any skin rashes or bites on your body?
Other resources:
Ticks Information Centre – Centers for Disease Control and Prevention
How keeping a travel history could save your life - Isabel Healthcare Blog
Could I have Lyme Disease – Patient information – Isabel Healthcare Blog
Have you read our white paper on why and how to improve diagnosis? Select the button below to download the white paper now.

Mandy Tomlinson
Mandy has worked for Isabel Healthcare since 2000. Prior to this, she was a Senior Staff Nurse on the Pediatric Infectious disease ward and high dependency unit at one of London's top hospitals, St Mary’s in Paddington which is part of Imperial College Healthcare NHS Trust. Her experience in the healthcare industry for the past 33 years in both the UK and USA means she's a vital resource for our organization. Mandy currently lives and works in Scottsdale, Arizona.
Subscribe Here!
Recent Posts
Meningococcal Infections: The Ongoing Need for Early Diagnosis in the UK (2026 Update)
Meningococcal infections (including meningococcal meningitis, meningococcal septicaemia, and..Isabel DDx Companion with ChatGPT Integration - to help you diagnose even faster
At Isabel Healthcare, we’ve always been driven by one goal: to make clinical reasoning faster,..List Of Categories
- Differential Diagnosis Decision Support
- Differential diagnosis
- Symptom Checker
- Symptoms
- Patient Disease Information
- Medical Error
- Disease
- Clinical Decision Support
- Diagnostic Decision Support
- Isabel 1 Minute Read
- Diagnosis Error
- Diagnosis Skills Cases
- Healthcare Informatics
- Clinical Reasoning
- Evidence-based Medicine
- Medical Education
- Patient Engagement
- Symptom Triage
- Nurse Practitioner Education
- Nursing Decision Support
- Partnership
- Public Health
- COVID-19
- EHR
- Patient Empowerment
- Patient Safety
- rare disease

Start your FREE Trial today
Try the Isabel Pro DDx generator for 30-days - no payment card details required.




