- Privacy Policy
- Terms & Conditions
- Contact us
- ©Isabel Healthcare 2025
What is chronic pelvic pain? Pelvic pain symptoms and causes
Chronic pelvic pain is pain in the pelvic area (below your belly button and above your hips) which lasts 6 months or longer and is affecting your quality of life. It affects 15-20% of women of reproductive age. Chronic pelvic pain can be intermittent or constant and it may present as a dull ache or it can be sharp. There may be a pattern to when chronic pelvic pain develops if its related to menstruation (monthly period/menses), it may occur before or after eating (postprandial), whilst passing urine, or maybe during sexual intercourse. Chronic pelvic pain is difficult to diagnose, treat and cure and so is a frustrating symptom for patient and doctor.
Causes of Chronic Pelvic PainChronic pelvic pain can be a symptom, or it can be caused by a variety of conditions. A symptom checker like Isabel can help you find information on common causes of chronic pelvic pain. Deciding what is causing your chronic pain will be a process of elimination performed by your doctor. Your doctor will take a detailed history of your pain, your health and family history. The doctor will then discuss some tests or exams with you, which will help them rule in or rule out conditions which could be causing you pelvic pain. These may include:
- Pelvic examination - Look for growths and signs of infection
- Lab tests – To check for bacterial infections and to check your blood counts.
- Ultrasound – Images of the internal structures of the body give precise information on the ovaries, uterus and fallopian tubes.
Other tests which may be performed include MRI, CT scans and laparoscopy.
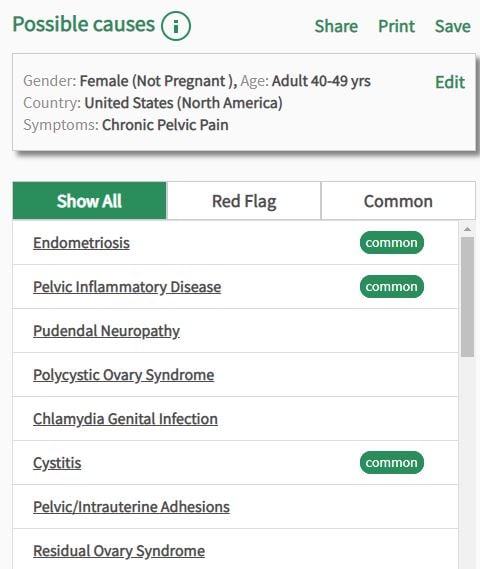 Isabel Symptom Checker – Chronic pelvic pain causes
Isabel Symptom Checker – Chronic pelvic pain causes
Further information on the causes of chronic pelvic pain conditions and other symptoms associated with these conditions in women include:
Endometriosis
If uterine tissue grows in other parts of the body such as the ovaries, pelvis or bladder then endometriosis can result. When a woman has her monthly period this tissue in other areas of the body can swell and bleed just as the uterine tissue does, which can cause chronic pelvic pain and scar tissue within the pelvic area. Symptoms include lower abdominal pain, painful periods, pain during or after sexual intercourse and an urgent need to pass urine. We have previously written about Endometriosis if you require further information on this condition.
Pelvic Inflammatory Disease (PID)
This is an infection within the female reproductive organs and can occur in the uterus, fallopian tubes or the ovaries. Several types of bacteria can cause PID including those that are sexually transmitted (Gonorrhea or Chlamydia). The bacteria normally enter the vagina and if left untreated can spread to the reproductive system, causing the infection to spread and symptoms to worsen. Symptoms include pelvic pain, fever, painful sexual intercourse, painful urination, irregular periods and vaginal discharge. As bacteria is the cause of this condition, antibiotics will be needed to treat the infection and prevent further complications from developing.
Uterine fibroids (uterine myoma)
These are non-cancerous growths, benign tumors, in the muscular wall of the uterus and can vary in size from tiny to large. Some women can have no symptoms with uterine fibroids, but it does depend on the size and location of the fibroids within the uterus. If they are large and close to other pelvic organs then symptoms experienced can include abnormal vaginal bleeding, stomach pain and a feeling of pressure within the stomach.
Pelvic Adhesions
These are caused by scar tissue, which sticks to organ and body tissues after surgery, infection, trauma or radiation and is found within the female reproductive organs, including the ovaries and fallopian tubes. Symptoms include pelvic pain, infertility, painful sexual intercourse or bowel obstruction.
Irritable bowel syndrome (IBS)
This is a very painful problem originating from the intestines. In IBS, the intestines will squeeze too hard or not hard enough, which causes the food to move too quickly or too slowly as it progresses through the intestines. Symptoms include lower abdominal pain, abdominal bloating, constipation and/or diarrhea.
Interstitial cystitis
This is a chronic condition that can cause pelvic pain, ranging from mild discomfort to severe pain. Other symptoms include bladder pressure, bladder pain and the frequent need to pass urine. Pelvic pain may also be experienced during sexual intercourse.
Talking to your doctor
Before your consultation with your doctor, think about the following questions they may ask you. It may also be helpful to keep a diary documenting your pelvic pain episodes to share with your doctor.
- How would you describe your pelvic pain?
- How long have you had the pelvic pain?
- Is the pelvic pain intermittent or persistent?
- What other symptoms do you have?
- Does anything alleviate the pelvic pain?
Finding the underlying cause of chronic pelvic pain can be a long process but working with your doctor to collect information about your symptoms can help work out a plan which enables you to treat the underlying cause, control your symptoms, and live an active life.
If any of the symptoms in this blog are concerning you, place them in the Isabel Symptom Checker and review the results with your doctor.

Mandy Tomlinson
Mandy has worked for Isabel Healthcare since 2000. Prior to this, she was a Senior Staff Nurse on the Pediatric Infectious disease ward and high dependency unit at one of London's top hospitals, St Mary’s in Paddington which is part of Imperial College Healthcare NHS Trust. Her experience in the healthcare industry for the past 33 years in both the UK and USA means she's a vital resource for our organization. Mandy currently lives and works in Scottsdale, Arizona.
Subscribe Here!
Recent Posts
Meningococcal Infections: The Ongoing Need for Early Diagnosis in the UK (2026 Update)
Meningococcal infections (including meningococcal meningitis, meningococcal septicaemia, and..Isabel DDx Companion with ChatGPT Integration - to help you diagnose even faster
At Isabel Healthcare, we’ve always been driven by one goal: to make clinical reasoning faster,..List Of Categories
- Differential Diagnosis Decision Support
- Differential diagnosis
- Symptom Checker
- Symptoms
- Patient Disease Information
- Medical Error
- Disease
- Clinical Decision Support
- Diagnostic Decision Support
- Isabel 1 Minute Read
- Diagnosis Error
- Diagnosis Skills Cases
- Healthcare Informatics
- Clinical Reasoning
- Evidence-based Medicine
- Medical Education
- Patient Engagement
- Symptom Triage
- Nurse Practitioner Education
- Nursing Decision Support
- Partnership
- Public Health
- COVID-19
- EHR
- Patient Empowerment
- Patient Safety
- rare disease

Start your FREE Trial today
Try the Isabel Pro DDx generator for 30-days - no payment card details required.




