- Privacy Policy
- Terms & Conditions
- Contact us
- ©Isabel Healthcare 2025
Types of Dementia - 1 Minute Read
 Dementia is not actually a specific disease, but rather a term that describes the significant loss of cognitive functioning and intellectual abilities which are severe enough to interfere with a person’s social or occupational functioning.
Dementia is not actually a specific disease, but rather a term that describes the significant loss of cognitive functioning and intellectual abilities which are severe enough to interfere with a person’s social or occupational functioning.
For dementia to be considered there should be impairment in two or more of the following areas:
- memory
- language
- abstract thinking
- praxis
- visuospatial or perceptual skills
- executive function
- personality
- social behavior
Dementia affects 1% of the population who are over 60 years of age and 40% of people who are over 85 years of age.
History and Medical Examination
A thorough examination is needed in order to identify dementia and then progress to identifying the medical condition which is causing the dementia. Take a history from the patient and a relative or carer. This includes:
- Asking about memory problems – do they forget names of friends and family? Can they recall recent events?
- Assessing activities of daily living – are they having problems working or carrying out everyday tasks. Can they operate phones or technology within the home? Can they make everyday decisions regarding finances or driving a car? Are they able to dress themselves and carry out their own hygiene requirements?
- Determining risk factors - enquire about cardiovascular and cerebrovascular risk factors, alcohol intake, medications they are taking and if any family members have been diagnosed with a type of dementia.
- Assessing their gait – do they have gait apraxia or gait ignition failure?
- Identifying if any focal neurological signs are present including hemiparesis, visual field defect and primitive reflexes
- Carrying out a thorough cognitive examination and identify deficits - are they able to hold a conversation with ease? Look for the patient using the ‘head-turning sign’ where they look to a care giver to answer a question for them.
- Testing executive function and see if there are any planning and organizing deficits present.
Lab Tests Needed
First-line investigations include FBC, ESR and routine chemistry. Consider obtaining thyroid function tests and checking vitamin B12 levels. Investigating sexually transmitted disease possibilities is important, particularly as these are often overlooked in the older generation, but are on the rise in the age group who are more at risk of developing dementia. Second-line investigations to be considered for suspected dementia include CSF beta amyloid and tau proteins, HIV testing, EEG, MRI and Single photon emission computed tomography (SPECT).
Dementia Differential Diagnosis
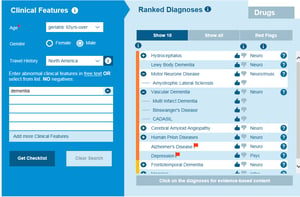
There is no single test that can conclusively diagnose one type of dementia from another. To diagnose exactly what type of dementia a patient has involves starting with the comprehensive history and physical examination which will identify the patient has a form of dementia. You then need to drill down and examine in detail what symptoms the patient has and identify the type of dementia they have based on clinical diagnosis. Each type of dementia has specific nuances that will help to identify the specific type of diagnosis. A differential diagnosis generator like the Isabel DDx Generator will help you research your patient’s individualized symptoms and drill down your differential. We have outlined some of the most common types and causes of dementia below.
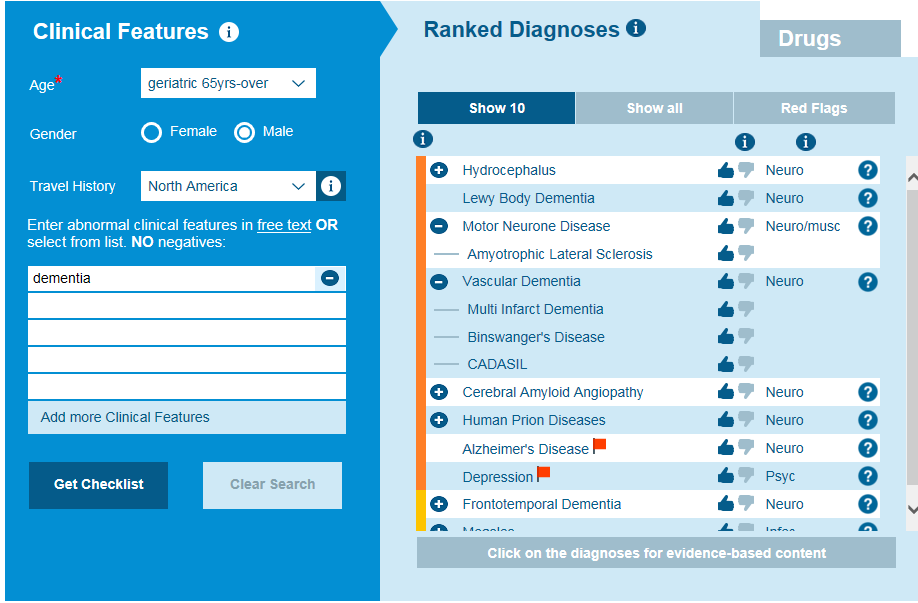
Isabel differential diagnosis for dementia
Lewy body dementia
This presents with dementia manifesting as changes in thinking and reasoning, confusion, slowness, gait imbalance and other parkinsonian movement symptoms. Patients may also have well-formed visual hallucinations, delusions and sleep disturbances. This commonly presents in elderly patients. If the patient has both dementia symptoms and movement symptoms at the time of diagnosis or if dementia symptoms appear within one year after movement symptoms, then the diagnosis is Lewy body dementia. Lewy body dementia can only be conclusively diagnosed on post mortem so judgement is a clinical one. It should be noted that Lewy bodies can coexist with Alzheimer’s brain changes and it can be hard to distinguish Lewy body dementia from Alzheimer’s disease.
Vascular dementia
This type of dementia occurs in patients over 40 years of age and risk factors include hypertension, smoking and vascular disease. The symptoms of vascular dementia can vary widely depending on the part of the brain which is affected. Clinical features include recurrent stepwise deterioration, pyramidal signs, pseudobulbar palsy, parkinsonism, gait disorder, confusion, disorientation and vision loss. Memory loss may not be a significant feature, as it depends on the specific brain area where blood flow is reduced and, therefore, symptoms vary with the individual. These changes can happen at the same time as physical stroke symptoms of headache, difficulty walking or numbness. They can also occur at the same time as multiple small strokes over a time period, causing a more gradual clinical picture with early symptoms of impaired judgement, inattention and difficulty finding the right words.
Alzheimer’s disease
This is commonly seen in people over 65 years of age. One of the most common early signs is short term memory loss, forgetting events or important dates and repeatedly asking for the same information. There may be changes in the person’s ability to plan and problem solve so early manifestations may include difficulty with keeping track of finances or time. Completing everyday tasks may become difficult, and other symptoms such as misplacing items, poor judgement, difficulty speaking or writing, changes in mood and personality are all signs that Alzheimer’s may be present.
Frontotemporal dementia
This has a usual onset of between 45-65 years. The nerves are damaged in the front regions of the brain and these cause behavior and personality changes and difficulty comprehending language. There are three subtypes of frontotemporal dementia known as:
- Behavioural variant FTD (bvFTD)
- Progressive non-fluent aphasia (PNFA)
- Semantic dementia (SD)
Diagnosing a specific type of dementia can be very challenging and it’s important to thoroughly evaluate the patient and rule out infections, depression, and seizures and other causes which are not dementia related and could be causing similar symptoms but are treatable and reversible. Dementia is a irreversible illness and it’s important to accurately diagnose the specific form of dementia on clinical judgement, using results of examinations and tests conducted and a differential diagnosis. Where possible treatment options can be prescribed to slow down the progression of the illness and enable the patient to maintain the best quality of life for as long as possible.

Mandy Tomlinson
Mandy has worked for Isabel Healthcare since 2000. Prior to this, she was a Senior Staff Nurse on the Pediatric Infectious disease ward and high dependency unit at one of London's top hospitals, St Mary’s in Paddington which is part of Imperial College Healthcare NHS Trust. Her experience in the healthcare industry for the past 33 years in both the UK and USA means she's a vital resource for our organization. Mandy currently lives and works in Scottsdale, Arizona.
Subscribe Here!
Recent Posts
Meningococcal Infections: The Ongoing Need for Early Diagnosis in the UK (2026 Update)
Meningococcal infections (including meningococcal meningitis, meningococcal septicaemia, and..Isabel DDx Companion with ChatGPT Integration - to help you diagnose even faster
At Isabel Healthcare, we’ve always been driven by one goal: to make clinical reasoning faster,..List Of Categories
- Differential Diagnosis Decision Support
- Differential diagnosis
- Symptom Checker
- Symptoms
- Patient Disease Information
- Medical Error
- Disease
- Clinical Decision Support
- Diagnostic Decision Support
- Isabel 1 Minute Read
- Diagnosis Error
- Diagnosis Skills Cases
- Healthcare Informatics
- Clinical Reasoning
- Evidence-based Medicine
- Medical Education
- Patient Engagement
- Symptom Triage
- Nurse Practitioner Education
- Nursing Decision Support
- Partnership
- Public Health
- COVID-19
- EHR
- Patient Empowerment
- Patient Safety
- rare disease

Start your FREE Trial today
Try the Isabel Pro DDx generator for 30-days - no payment card details required.




