- Privacy Policy
- Terms & Conditions
- Contact us
- ©Isabel Healthcare 2025
Loss of Appetite or Anorexia | 1 Minute Read | Isabel Healthcare
 Anorexia is defined as the decreased sensation of appetite or loss of appetite and the terms can be used interchangeably. This is not to be confused with the eating disorder anorexia nervosa, which will be discussed as a possible reason for this symptom. Loss of appetite is a symptom which can occur in many diseases and its presence can raise alarm bells and red flags in some diseases both physical and psychological.
Anorexia is defined as the decreased sensation of appetite or loss of appetite and the terms can be used interchangeably. This is not to be confused with the eating disorder anorexia nervosa, which will be discussed as a possible reason for this symptom. Loss of appetite is a symptom which can occur in many diseases and its presence can raise alarm bells and red flags in some diseases both physical and psychological.
What is Hunger and Appetite
The feelings of hunger and its opposite satiety are regulated by complex mechanisms in the body. Hunger originates in the stomach, and here a hormone called ghrelin is released when blood sugar and insulin levels drop. This hormone then communicates with the hypothalamus in the brain to trigger the feeling we know as hunger. The hypothalamus regulates the body’s basic body functions such as thirst, sleep and sex drive. The hypothalamus receives a message from ghrelin that the body needs food to keep running efficiently and the hypothalamus releases neuropeptide Y which then stimulates the body’s appetite.
Accurate history taking
Loss of appetite may only present itself as a symptom when you are discussing other symptoms with your patient. You should determine what is a normal appetite for the patient and if they state they have loss of appetite determine over what time they have noticed their appetite has been decreasing. Also, determine if anything has changed in their life recently which may have led to their appetite decreasing. Asking the patient to keep a food diary recording what they eat each day, and also asking how they feel before they eat and after they eat may be helpful. Ask them whether they have any other symptoms that stop the patient eating like dysphagia, odynophagia or epigastric reflux.
Ensure you perform a full physical examination of the patient, looking for signs of cachexia and considering psychological symptoms including cognitive impairment or flat affect. Weigh the patient and calculate an accurate BMI and compare with any previous values in their medical record.
Differential diagnosis
Loss of appetite has a wide differential diagnosis which is why it is important to establish when the loss of appetite occurred and if other symptoms are present to narrow down the differential diagnosis.
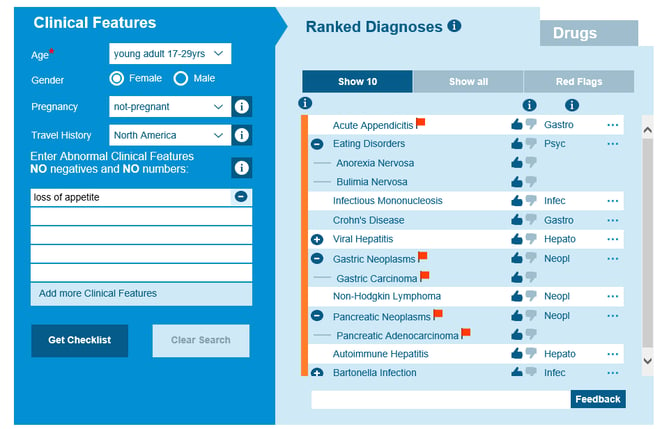
Differential diagnosis of loss of appetite is broad
If the loss of appetite has occurred recently and there are symptoms of an acute infection, then their appetite should return when the infection subsides.
Acute appendicitis
This should be considered in any patient presenting with abdominal pain, nausea or vomiting as well as loss of appetite. Symptoms develop quickly and as it is a ‘don’t miss diagnosis’ the patient should be evaluated quickly to determine if present and prevent further complications occurring.
Anorexia nervosa
Anorexia nervosa is not caused directly by a loss of appetite, as people with this disorder intentionally avoid eating to prevent weight gain. However, the patient’s relationship with food can lead to a psychological loss of appetite, and as they eat lessl, the body responds with a decreased appetite in an effort to continue running as best as it can. It is important to establish the patient’s relationship with food in your history taking.
Psychological causes
Disorders which are not necessarily eating disorders but which have psychological origins, such as depression, can affect the appetite. Patients with depression can forget to eat or may lose interest in food. Symptoms indicating a psychological aetiology may include:
- persistent low mood
- anergia
- loss of concentration
- anhedonia
- helplessness
- hopelessness
- excess alcohol intake
- memory disturbance
Crohn’s disease
Many reasons for loss of appetite can be caused by this disease. Other symptoms of Crohn’s disease include nausea, abdominal pain, bloating and diarrhea, which can all make the person feel less like eating as they know eating will exacerbate these symptoms and the disease. Many patients also suffer from mouth ulcers which can prevent people from eating. Finally, fatigue caused by Crohn’s disease can mean people won’t prepare healthy meals or do not have the energy to eat properly.
Malignancies
Loss of appetite which has occurred over a prolonged period could indicate an underlying malignancy. It is particularly common in patients who are diagnosed with solid tumor cancers including breast and lung cancer. Weight loss often occurs when a cancer spreads to the liver and impairs its functioning especially when regulating appetite and removing toxins. Weight loss can be an early sign of colon cancer. Losing significant weight such as 10 pounds a month or 10% of a patient’s weight in a span of six months is a cause for concern and malignancy should be considered when seeking out additional symptoms.
Investigations and Tests
To thoroughly investigate the disease causes of a patient’s loss of appetite the following should be actioned:
- blood tests
- helicobacter pylori stool antigen
- chest x-ray if respiratory symptoms are also present
- abdominal ultrasound
- depression screening
- alcohol-use questionnaire
- mini mental state examination (MMSE) to evaluate cognitive function
- if reflux disease is suspected then an endoscopy may be needed
- if malignancy is suspected then investigations into the lower GI tract may be required
Loss of appetite has many causes and due to this it is important that this symptom is thoroughly investigated with an accurate work up. If not detected then consequences of loss of appetite can include muscle wasting, decreased immunocompetence, depression and an increased rate of disease complications. A strong correlation exists between weight loss and associated morbidity and mortality so it’s important when a patient presents with this symptom that they are thoroughly examined and all possible causes are considered in their differential diagnosis until a cause is found.
Try Isabel for free to see how it can help with your differential diagnosis:
Image Attribution:
"Wall_Food_10139" (CC BY-SA 2.0) by Michael Stern

Mandy Tomlinson
Mandy has worked for Isabel Healthcare since 2000. Prior to this, she was a Senior Staff Nurse on the Pediatric Infectious disease ward and high dependency unit at one of London's top hospitals, St Mary’s in Paddington which is part of Imperial College Healthcare NHS Trust. Her experience in the healthcare industry for the past 33 years in both the UK and USA means she's a vital resource for our organization. Mandy currently lives and works in Scottsdale, Arizona.
Subscribe Here!
Recent Posts
Meningococcal Infections: The Ongoing Need for Early Diagnosis in the UK (2026 Update)
Meningococcal infections (including meningococcal meningitis, meningococcal septicaemia, and..Isabel DDx Companion with ChatGPT Integration - to help you diagnose even faster
At Isabel Healthcare, we’ve always been driven by one goal: to make clinical reasoning faster,..List Of Categories
- Differential Diagnosis Decision Support
- Differential diagnosis
- Symptom Checker
- Symptoms
- Patient Disease Information
- Medical Error
- Disease
- Clinical Decision Support
- Diagnostic Decision Support
- Isabel 1 Minute Read
- Diagnosis Error
- Diagnosis Skills Cases
- Healthcare Informatics
- Clinical Reasoning
- Evidence-based Medicine
- Medical Education
- Patient Engagement
- Symptom Triage
- Nurse Practitioner Education
- Nursing Decision Support
- Partnership
- Public Health
- COVID-19
- EHR
- Patient Empowerment
- Patient Safety
- rare disease

Start your FREE Trial today
Try the Isabel Pro DDx generator for 30-days - no payment card details required.




