- Privacy Policy
- Terms & Conditions
- Contact us
- ©Isabel Healthcare 2025
IBD vs IBS - What’s the difference?
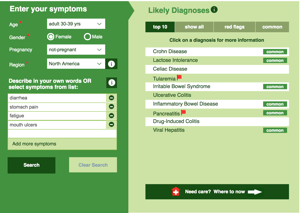 In the world of digestion there are many terms and different conditions, and so it’s no wonder that this can cause some confusion. The symptoms for many gastrointestinal conditions, as they are known, can be quite similar as well, and this can lead to misdiagnosis or delayed diagnosis. Two very common terms we hear around the subject are ‘IBD’ and ‘IBS.’ You’d be forgiven for thinking these two acronyms are interchangeable and refer to the same condition, but they are, in reality, different. We will explain the two terms in this blogpost, talk about some of the symptoms of common gastrointestinal conditions, and the treatments that are recommended for them.
In the world of digestion there are many terms and different conditions, and so it’s no wonder that this can cause some confusion. The symptoms for many gastrointestinal conditions, as they are known, can be quite similar as well, and this can lead to misdiagnosis or delayed diagnosis. Two very common terms we hear around the subject are ‘IBD’ and ‘IBS.’ You’d be forgiven for thinking these two acronyms are interchangeable and refer to the same condition, but they are, in reality, different. We will explain the two terms in this blogpost, talk about some of the symptoms of common gastrointestinal conditions, and the treatments that are recommended for them.
What is IBD? Inflammatory Bowel Disease
IBD can be used to mean Ischemic Bowel Disease, but that's for another blogpost. In this blogpost we will focus on Inflammatory Bowel Disease, which is in fact an umbrella term for a range of gastrointestinal diseases which involve inflammation of the digestive or gastrointestinal (GI) tract. The two main conditions that are considered to be inflammatory bowel diseases are ulcerative colitis and Crohn’s disease.
Ulcerative colitis
Ulcerative colitis occurs in the colon, which is the large intestine leading into the rectum. Ulcers and sores can develop in the lining of the colon and rectum, causing pain, bleeding or infection. There are periods of time when symptoms are worsened, known as flare ups, and the cause is unknown, although we do think it is an autoimmune condition, meaning the body wrongly attacks healthy bacteria and cells by mistake. The main symptoms of ulcerative colitis are:
- Chronic diarrhea
- Blood, mucus or pus in feces
- Abdominal pain, often quite low down nearer the rectum
- Fatigue
- Weight loss
- Loss of appetite
In addition to these direct symptoms, during a flare up some people can experience the following:
- Mouth Ulcers
- Arthritis
- Irritation to the skin
- Irritation to the eyes
Crohn’s disease
Crohn’s disease affects around 1.6 million americans and is a chronic condition with periods of remission and flare ups, similar to ulcerative colitis. The difference here however, is that Crohn’s disease occurs when any part of the digestive tract becomes inflamed. They are not necessarily sores, and flare ups can range from slight irritation to excruciating pain. We are also even less sure of the causes of Crohn’s disease than we are for ulcerative colitis, but genes and the immune system are thought to potentially have something to do with it. The symptoms of Crohn’s disease during a flare up are similar to ulcerative colitis:
- Chronic diarrhea
- Blood in feces
- Abdominal pain and cramps
- Fatigue
- Weight loss
- Loss of appetite
Treatment for both ulcerative colitis and Crohn’s disease are similar, and usually involve aminosalicylates (5-ASAS) or steroids which both work to control inflammation, and immunosuppressants to help the immune system stop attacking healthy bacteria in the digestive tract. In some cases, particularly with children, liquid food is used to help reduce inflammation and stop flare ups. Once in remission, these treatments are often continued to maintain remission, and diet is often looked at as individuals may have different dietary triggers. If the condition is not improving sometimes surgery is offered to remove a section of intestine that is particularly inflamed. This is usually done as keyhole surgery, and sometimes requires an ileostomy, where feces bypass the colon and/or rectum and go into a bag, whilst the digestive system heals from the surgery.
What is IBS? Irritable Bowel Syndrome
So now we know what IBD means and some of the more common conditions within this. So what is IBS? Irritable Bowel Syndrome is actually not considered a disease, but is referred to as a functional disorder. This means it is a condition without an identifiable cause. There is no inflammation seen in the digestive system, but there are physical symptoms which suggest discomfort or irritation when digesting, making it hard to trace and even harder to treat. IBS is a very common condition, with as many as 45 million people in the US suffering at some point in their life. Symptoms can include:
- Abdominal pain or cramps
- Diarrhea
- Constipation
- Bloating
- Nausea
- Fatigue
- Backache
- Urination issues
- Incontinence
Treatment for IBS is mainly dietary and can be different for everyone. Mostly people tend to be able to control flare ups by generally improving their diet to a more healthy one, cutting out fatty, spicy, or processed foods. Some find cutting out allergens such as lactose or wheat can help with symptoms, as well as increasing fluid intakes and making sure meals aren’t missed. Preventing flare ups can be controlled in the same way, as well as considering other causes and trigger; some people consider stress or tiredness to be a trigger for IBS flareups, so managing these triggers can help.
If you are experiencing any symptoms mentioned in this blogpost, or think you may have a gastrointestinal condition, place everything into the Isabel Symptom Checker and discuss the results and treatment options with your doctor.

Mandy Tomlinson
Mandy has worked for Isabel Healthcare since 2000. Prior to this, she was a Senior Staff Nurse on the Pediatric Infectious disease ward and high dependency unit at one of London's top hospitals, St Mary’s in Paddington which is part of Imperial College Healthcare NHS Trust. Her experience in the healthcare industry for the past 33 years in both the UK and USA means she's a vital resource for our organization. Mandy currently lives and works in Scottsdale, Arizona.
Subscribe Here!
Recent Posts
Meningococcal Infections: The Ongoing Need for Early Diagnosis in the UK (2026 Update)
Meningococcal infections (including meningococcal meningitis, meningococcal septicaemia, and..Isabel DDx Companion with ChatGPT Integration - to help you diagnose even faster
At Isabel Healthcare, we’ve always been driven by one goal: to make clinical reasoning faster,..List Of Categories
- Differential Diagnosis Decision Support
- Differential diagnosis
- Symptom Checker
- Symptoms
- Patient Disease Information
- Medical Error
- Disease
- Clinical Decision Support
- Diagnostic Decision Support
- Isabel 1 Minute Read
- Diagnosis Error
- Diagnosis Skills Cases
- Healthcare Informatics
- Clinical Reasoning
- Evidence-based Medicine
- Medical Education
- Patient Engagement
- Symptom Triage
- Nurse Practitioner Education
- Nursing Decision Support
- Partnership
- Public Health
- COVID-19
- EHR
- Patient Empowerment
- Patient Safety
- rare disease

Start your FREE Trial today
Try the Isabel Pro DDx generator for 30-days - no payment card details required.




