- Privacy Policy
- Terms & Conditions
- Contact us
- ©Isabel Healthcare 2025
Could I have osteoporosis? Osteoporosis signs and symptoms
 20 October is World Osteoporosis Day, calling for global action to help improve bone health and prevent fractures caused by this condition that, much too often, is diagnosed too late to make a difference. Osteoporosis is a growing problem around the world affecting one in three women and one in five men over the age of 50. Fractures caused by osteoporosis can have a devastating impact, not only on the sufferer but on costs to society and healthcare systems. And yet despite effective medical advances, only 10% of women with fractures will receive osteoporosis therapy. In 2010 in Europe alone it was estimated that 12.3 million high-risk patients were left untreated. Increased awareness is undoubtedly the key, both among the medical profession and among patients who should look out for the early warning signs and make lifestyle choices to help prevent osteoporosis from defining their old age.
20 October is World Osteoporosis Day, calling for global action to help improve bone health and prevent fractures caused by this condition that, much too often, is diagnosed too late to make a difference. Osteoporosis is a growing problem around the world affecting one in three women and one in five men over the age of 50. Fractures caused by osteoporosis can have a devastating impact, not only on the sufferer but on costs to society and healthcare systems. And yet despite effective medical advances, only 10% of women with fractures will receive osteoporosis therapy. In 2010 in Europe alone it was estimated that 12.3 million high-risk patients were left untreated. Increased awareness is undoubtedly the key, both among the medical profession and among patients who should look out for the early warning signs and make lifestyle choices to help prevent osteoporosis from defining their old age.
What is osteoporosis?
Osteoporosis is a condition that weakens the bones making them fragile and consequently more likely to break or fracture. The condition doesn’t come on suddenly but develops over a period of time. Bones are at their thickest and strongest early on in your adult life. We gradually start to lose bone density around the age of 35. This happens to everyone but for some it happens much more quickly. The condition currently affects over 44 million in the US and more than 3 million in the UK.
Symptoms and signs of osteoporosis
- Many patients won’t experience any symptoms or know they’ve got Osteoporosis until they break a bone for no obvious reason such as a sudden impact or minor fall. The most common injuries in sufferers are wrist and hip fractures and fractures in the vertebrae or spinal column. But the condition can affect other areas; something as simple as a sneeze is sometimes enough to cause a rib fracture
- Some older sufferers develop a characteristic stooped posture as a result of fractures in the spinal column which make it difficult to support body weight
- Receding gums can be attributed to a variety of factors, one of which is osteoporosis. Our teeth are connected to the jaw bone and if the jaw is losing bone, gums can recede
- In postmenopausal women handgrip strength is an important test factor related to overall bone mineral density
- Weak or brittle fingernails may indicate poor bone density
- Bone and muscle aches. As they are often associated with the ageing process, they are commonly overlooked but could be a sign of Vitamin D deficiency. Similarly, cramping in the leg can be associated with poor calcium and magnesium levels which in turn can lead to excessive bone loss.
Who is it at risk of osteroperosis?
- Women in the first few years after the menopause are more at risk, particularly if their menopause begins before 45. This is due to the fall in oestrogen levels which is needed for healthy bones
- Women who’ve had a hysterectomy before the age of 45
- A family history of the disease, and in particular a hip fracture in a parent
- Long-term use of particular medications, notably steroids and certain cancer treatments
- Those suffering from certain medical conditions, namely inflammatory or malabsorption conditions such as coeliac disease and Crohn’s; also hormone-related illnesses such as hyperthyroidism
- People with a low body mass index (BMI)
- Heavy drinkers and smokers
- Men with low testosterone levels
- Sufferers of eating disorders such as anorexia or bulimia
Diagnosis of osteoporosis
If your doctor suspects Osteoporosis, you may be referred for further assessment or a scan which measures your bone density. Tests may reveal you are instead suffering from Osteopenia which indicates a decrease in bone density but is not enough to be classed as Osteoporosis.
Treatment for osteoporosis
Osteoporosis treatment centres around preventing further fractures and using medication to strengthen bones. Your treatment plan will depend on many factors such as your age, previous history of injury and your risk of further fractures. Current treatments include Bisphosphonates which are designed to slow down the rate the bone is broken down in your body. Some patients are offered SERMs (Selective Oestrogen Receptor Modulators) which act like the oestrogen hormone in helping to maintain bone density. Parathyroid hormone treatments are also offered to stimulate cells to create new bone, as is HRT (Hormone Therapy treatment) to women going through the menopause.
Prevention of osteoporosis
While our genes are responsible for determining the height and strength of our skeleton, it is most commonly our lifestyle choices which influence the health of our bones. There are a lot of lifestyle changes we can make to stave off or hopefully prevent the onset of this debilitating condition:
- Healthy Eating: Calcium and Vitamin D are vital for maintaining strong bones, so make sure you include some of the following in your daily diet:
- Leafy green vegetables
- Dried fruit
- Yoghurt
- Tofu
- Oily fish
- Red meat
- Egg yolks
- Quit smoking and drinking, both of which are linked to an increased risk of osteoporosis
- Get lots of sunshine! Not always easy in certain parts of the northern hemisphere, especially in the winter months, but from March to September, short periods spent outside without sunscreen between the hours of 11am-3pm (depending on where you live) should be enough to boost your Vitamin D levels. Clearly care should be taken not to burn so make sure you apply suncream when the sun is hot. As a rule, the darker your skin, the longer it takes to absorb vitamin D. If you know you’re not getting enough time outside, taking supplements is advised. Using sunbeds is not a recommended way to make Vitamin D.
- Regular exercise: Adults between the ages of 19-64 should do at least 2 hours 30 minutes of moderate-intensity aerobic activity each week. Weight-bearing and resistance exercises are particularly important in improving bone density.
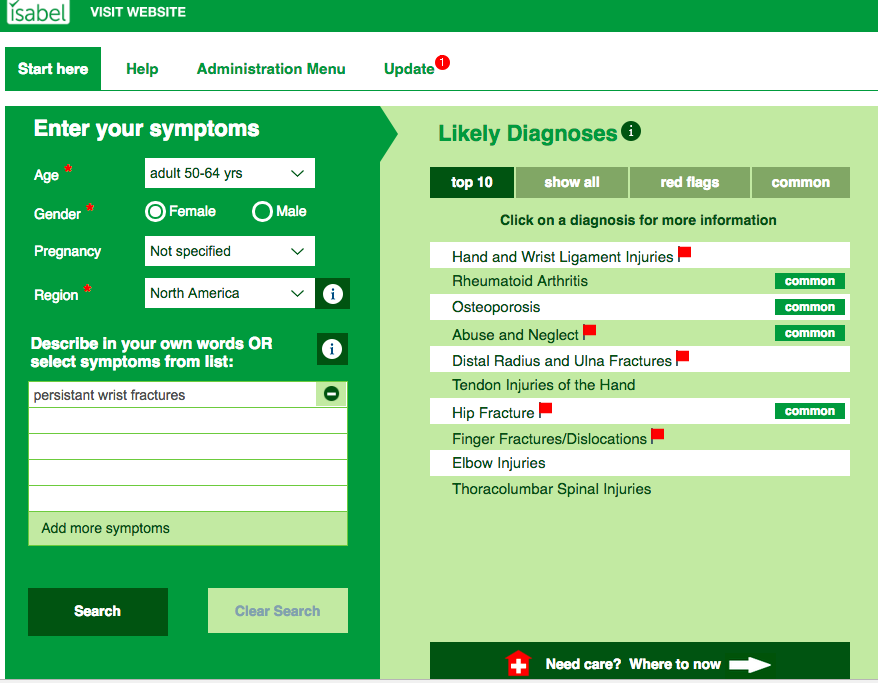
If, having read this blog, you suspect you could be a potential Osteoporosis sufferer, contact your doctor to see what action can be taken to help prevent the condition getting worse. You can also enter your symptoms into the Isabel Symptom Checker and discuss the results with your doctor.
Subscribe Here!
Recent Posts
Meningococcal Infections: The Ongoing Need for Early Diagnosis in the UK (2026 Update)
Meningococcal infections (including meningococcal meningitis, meningococcal septicaemia, and..Isabel DDx Companion with ChatGPT Integration - to help you diagnose even faster
At Isabel Healthcare, we’ve always been driven by one goal: to make clinical reasoning faster,..List Of Categories
- Differential Diagnosis Decision Support
- Differential diagnosis
- Symptom Checker
- Symptoms
- Patient Disease Information
- Medical Error
- Disease
- Clinical Decision Support
- Diagnostic Decision Support
- Isabel 1 Minute Read
- Diagnosis Error
- Diagnosis Skills Cases
- Healthcare Informatics
- Clinical Reasoning
- Evidence-based Medicine
- Medical Education
- Patient Engagement
- Symptom Triage
- Nurse Practitioner Education
- Nursing Decision Support
- Partnership
- Public Health
- COVID-19
- EHR
- Patient Empowerment
- Patient Safety
- rare disease

Start your FREE Trial today
Try the Isabel Pro DDx generator for 30-days - no payment card details required.




