- Privacy Policy
- Terms & Conditions
- Contact us
- ©Isabel Healthcare 2025
Could I have heart disease? CVD conditions, symptoms and causes
 Our blog this week is devoted to cardiovascular disease, or heart disease, to tie in with the new online ‘Heart Age Test’ recently launched by Public Health England (PHE) in the UK. PHE decided to launch the campaign to try and help reduce the number of people who die unexpectedly and unnecessarily each year from heart attacks and strokes. According to PHE, “Millions are at risk of cardiovascular disease but don’t know it, putting themselves at real risk of suffering ill health or dying younger”. While the death rate from cardiovascular disease has seen a massive drop, falling more than 75% since 1961, it still causes more than a quarter of all deaths in the UK with similar figures in the US.
Our blog this week is devoted to cardiovascular disease, or heart disease, to tie in with the new online ‘Heart Age Test’ recently launched by Public Health England (PHE) in the UK. PHE decided to launch the campaign to try and help reduce the number of people who die unexpectedly and unnecessarily each year from heart attacks and strokes. According to PHE, “Millions are at risk of cardiovascular disease but don’t know it, putting themselves at real risk of suffering ill health or dying younger”. While the death rate from cardiovascular disease has seen a massive drop, falling more than 75% since 1961, it still causes more than a quarter of all deaths in the UK with similar figures in the US.
Doing the test, which is aimed at those over 30 years of age, involves answering a few simple questions online, at the end of which you’ll be given your ‘heart age’. Of the 2 million people who have completed the test so far, 78% found their heart age to be higher than their actual age with 14% having a heart age of more than 10 years their real age. The test takes no more than a few minutes and can be done here.
What is heart disease?
Known in medical terms as Cardiovascular Disease (CVD), heart disease encompasses any condition affecting the heart or blood vessels. It is most commonly associated with the build-up of fatty deposits inside the arteries, the main blood vessels delivering oxygen-rich blood from the heart to all parts of the body. This in turn leads to an increased risk of blood clots. While there are many different types of heart disease, below are listed the four main types:
Coronary Heart Disease
This occurs when the flow of oxygen-rich blood to the heart is either reduced or blocked, putting an increased strain on the heart which then leads to one of the following:
Angina
The main symptom of Angina is chest pain. It’s not usually life-threatening but should be taken very seriously and seen as a warning sign to a potential heart attack or stroke
Heart failure
This doesn’t mean the heart has stopped; heart failure is considered a chronic condition meaning your heart needs support to help it work properly. It’s main symptoms are breathlessness, tiredness and often swollen legs and ankles.
Heart attack
This is the most serious of the three and requires immediate medical attention. Heart attacks are caused when the blood supply to the heart is suddenly blocked, usually by a blood clot. As a lack of blood to the heart can cause serious damage, time is of the essence and immediate action should be taken. The key symptoms of a heart attack are:
- chest pain - sufferers often describe a squeezing sensation with pain often radiating out to the jaw, arms and back
- shortness of breath
- nausea
- pains in other areas of the body, particularly travelling from the chest to the arms
- feeling panicked
Stroke and Transient Ischemic Attack (TIA)
A stroke is in fact a cardiovascular disease, as it involves the blood vessels and the way they travel to the brain. A stroke occurs when the blood supply to part of the brain is cut off causing brain damage and possibly death. Like the heart attack, this is a serious life-threatening condition requiring immediate medical treatment. An easy way to remember the key stroke symptoms is with the word F.A.S.T:
F for the patient’s face which may have dropped on one side, usually at either the eye or mouth.
A for arms which may feel numb or very weak.
S for speech which may be slurred or even non-existent, even though the patient is awake.
T for time: time is of the essence as the sooner the patient receives treatment, the less damage is likely to occur so dial your emergency number as soon as possible
A Transient Ischemic Attack (TIA) is also known as a mini-stroke, and occurs when blood flow to the brain is only temporarily disrupted. This blockage can cause the sudden onset of symptoms similar to a stroke but the symptoms will usually only last for a few minutes or hours. Nevertheless the F.A.S.T. rules as above should be applied as a TIA is often a warning that a full stroke is imminent.
Peripheral Arterial Disease (PAD)
Also known as Peripheral Vascular Disease, this occurs when there is a blockage in any of the arteries leading to the limbs, most commonly the legs. Most people will experience pain in their legs when walking, ranging from mild to severe. The pain most commonly disappears after a short rest. Other symptoms include weak or numb legs, leg ulcers that don’t heal, shiny skin, hair loss on legs and feet, and in men, erectile disfunction. These symptoms usually develop over a period of time but in some cases can develop quickly. Either way, you should visit your doctor as soon as you notice the symptoms.
Aortic disease
This is a group of conditions that affect the aorta, which is your largest blood vessel carrying blood from the heart to the rest of the body. The most commonly known of these conditions is the abdominal aortic aneurysm (AAA), which causes the aorta to bulge outwards, eventually bursting and causing life-threatening bleeding. The most common symptoms of AAA are persistent tummy pain and lower back pain, but many AAA’s don’t cause any symptoms and are only picked up during screening.
What causes CVD?
While the exact cause is unknown, and the different conditions may have different causes, there are many factors which play a role in increasing your risk of any of the above conditions, the main ones being:
- High Blood Pressure (or hypertension) - this rarely has symptoms but if left untreated, is a major cause of CVD. As more than 1 in 4 adults in the UK has high blood pressure, it’s good to ask for a test every so often from your doctor and even purchase a home blood pressure monitor kit so you can keep a regular eye on it.
- Smoking - this is due to the harmful substances in tobacco causing damage to your blood vessels
- High Cholesterol - cholesterol is a fatty substance found in your blood which, if high, can narrow the blood vessels leading to blood clots
- Diabetes - the high blood sugar levels caused by diabetes lead to the narrowing and damage of the blood vessels
- Being overweight or obese - this may lead to high blood pressure as well as diabetes, both of which are risk factors for CVD
- Family History - If a close member of your family, such as a parent or sibling, has had CVD, you are more at risk
- Your ethnic background - CVD is more common in people of South Asian, African and Caribbean background
- Excessive alcohol consumption - this can increase your cholesterol and blood pressure and lead to weight gain, all of which are risk factors for CVD.
If you do the Heart Age Test, you will be questioned about most of the risk factors mentioned above. And if you need any more encouragement to do the test, Public Health England has sobering words: “Knowing your heart age is a simple way of finding out whether you’re at risk of a heart attack or stroke. By making important lifestyle changes you can reduce your risk before it’s too late.”
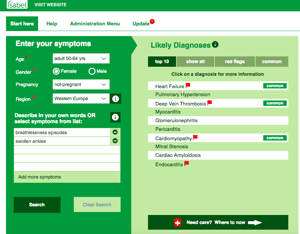
If you have any of the symptoms mentioned above, you can also enter them into the Isabel Symptom Checker and discuss the results with your doctor.
Subscribe Here!
Recent Posts
Meningococcal Infections: The Ongoing Need for Early Diagnosis in the UK (2026 Update)
Meningococcal infections (including meningococcal meningitis, meningococcal septicaemia, and..Isabel DDx Companion with ChatGPT Integration - to help you diagnose even faster
At Isabel Healthcare, we’ve always been driven by one goal: to make clinical reasoning faster,..List Of Categories
- Differential Diagnosis Decision Support
- Differential diagnosis
- Symptom Checker
- Symptoms
- Patient Disease Information
- Medical Error
- Disease
- Clinical Decision Support
- Diagnostic Decision Support
- Isabel 1 Minute Read
- Diagnosis Error
- Diagnosis Skills Cases
- Healthcare Informatics
- Clinical Reasoning
- Evidence-based Medicine
- Medical Education
- Patient Engagement
- Symptom Triage
- Nurse Practitioner Education
- Nursing Decision Support
- Partnership
- Public Health
- COVID-19
- EHR
- Patient Empowerment
- Patient Safety
- rare disease

Start your FREE Trial today
Try the Isabel Pro DDx generator for 30-days - no payment card details required.




