- Privacy Policy
- Terms & Conditions
- Contact us
- ©Isabel Healthcare 2025
Could I have Fibromyalgia? | FM symptoms and diagnosis
 The most common answer to this question is…. “possibly, but we can’t say for sure … come back in 3 months time.” Not what you want to hear when your body’s wracked with aches and pains, you’re depressed, exhausted, constipated and constantly getting migraine. Fibromyalgia (FM), a condition which causes chronic muscle pain throughout the body, is thought to affect 3-6% of the world’s population, which on first glance doesn’t seem like a large percentage. When you actually add up the math though, it means that 450 million people are diagnosed with FM, and a huge 75% of those people are female.
The most common answer to this question is…. “possibly, but we can’t say for sure … come back in 3 months time.” Not what you want to hear when your body’s wracked with aches and pains, you’re depressed, exhausted, constipated and constantly getting migraine. Fibromyalgia (FM), a condition which causes chronic muscle pain throughout the body, is thought to affect 3-6% of the world’s population, which on first glance doesn’t seem like a large percentage. When you actually add up the math though, it means that 450 million people are diagnosed with FM, and a huge 75% of those people are female.
There is, however, a further flaw in these statistics. FM is far from easy to diagnose, and a recent study concluded that two thirds of FM patients have been misdiagnosed with the condition, and could actually have something else. That’s 300 million people who have potentially been misdiagnosed with Fibromyalgia.
Why is FM so hard to diagnose?
Firstly, there’s no definitive blood test or x-ray to confirm the diagnosis. FM falls into the category of a 'diagnosis by exclusion,’ meaning doctors have to rule out all other possibilities before being able to label it as FM. The Center for Disease Control and Prevention bases its official FM diagnosis on “symptoms that have been present for at least 3 months,” adding that "the patient does not have [another] disorder that would otherwise explain the pain”. FM shares common symptoms with many other illnesses such as Chronic Fatigue Syndrome, Rheumatoid Arthritis and MS to name just a few, so you can see why the diagnostic process for FM can get tricky very easily.
Secondly, Fibromyalgia is a relative newcomer to the world of chronic illnesses. It was first classified in 1990 by the American College of Rheumatology, and according to many, the diagnostic criteria set out by the College was in itself flawed. The criteria was then reviewed again in 2010 so confusion among doctors and patients is understandably widespread, further complicating the diagnosis of this illness.
Fibromyalgia symptoms
- Widespread muscular aches and pains - Many patients describe how themselves as ‘hurting all over’. The pain can vary from burning or throbbing, to shooting pains, and can vary according to the time of the day, the weather, stress levels or the type of activity you may have done the day before
- Fatigue - The level and presentation of fatigue can be different for each patient. It can be mild in some, incapacitating in others, and some may feel utterly drained of energy, whilst others may feel mentally tired and struggle to concentrate for even a short time
- Sleep Disorder - The patient has interrupted levels of deep sleep (or stage 4 sleep), leaving them feeling exhausted despite having slept the whole night through. Insomnia and not sleeping at all is more rare in FM patients, although the pain keep them up sometimes
- Stiffness - Many patients complain of feeling particularly stiff in the morning or after long periods spent in the same position
- Irritable Bowel Syndrome - With symptoms ranging from constipation and diarrhoea to abdominal pain. IBS is another difficult condition to diagnose, and as such can complicate diagnosis of FM
- Cognitive problems - Often referred to as ‘Fibro Fog’, patients can have problems remembering or learning new things, or their speech might become slow and confused
- Chronic Headaches - Recurrent migraine and tension-type headaches which could be linked to pain and stiffness in the patient’s neck and shoulders
- Extreme Sensitivity - FM can make your body extremely sensitive to pain - even the slightest touch can be excruciating. The pain from a simple injury like stubbing your toe could last much longer than normal, and be more intense as well
- Sensitivity Syndrome - Heightened sensitivity to odours, noises, bright lights and certain foods.
These are just some of the main symptoms of FM, but the list goes on. From painful periods to numbness and tingling, the diverse range of symptoms make this a very difficult diagnostic process.
Causes of Fibromyalgia
The causes of FM are just as elusive as the diagnosis but there do seem to be common triggers.
- A viral or bacterial infection
- The development of another disorder such as rheumatoid arthritis, lupus or hypothyroidism
- Other aggravating factors include hormonal fluctuations such as the menopause, stress, depression and over-exertion
- An injury or major operation
- Bereavement or breakdown of a relationship
- Genetics: It's also suggested that some people are more likely to develop fibromyalgia because of genes inherited from their parents.
There is still a lot of research happening into the causes and treatment of FM, and one leading theory is about hormone levels. It is suggested that FM patients have developed changes in the way their central nervous systems process the pain messages from their brain due to a chemical inbalance. Research has shown that people with FM have abnormally low levels of the hormones serotonin, noradrenaline and dopamine: these hormones are vital for regulating your mood, appetite and sleep and are connected with the processing of pain messages from the brain.
How is FM diagnosed?
As a first step, put your symptoms into the Isabel Symptom Checker. However, even with the most common symptoms normally associated with FM you’ll notice the diagnosis doesn’t necessarily appear near the top of the list as you’ll see on this screenshot:
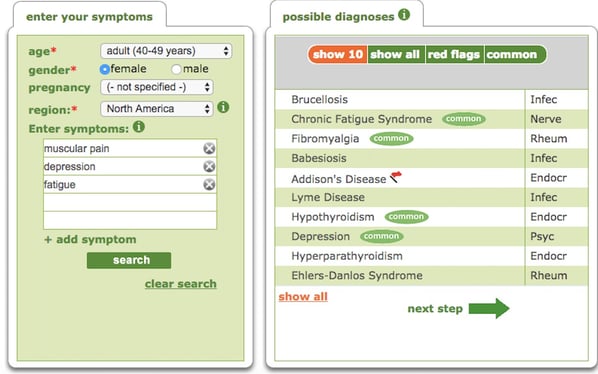
This reflects the point mentioned above that FM is frequently misdiagnosed in the place of other similar conditions (you may notice these appearing further up the list). Your Doctor may be able to immediately rule out some of the conditions on the list or may refer you to a specialist as it’s only when these other conditions which share FM’s symptoms have been dismissed that a diagnosis of FM can finally be made. That is why, particularly in these cases, symptom checkers and good communication with your doctor can help with diagnosis, and avoiding being wrongly diagnosed with Fibromyalgia.
Fibromyalgia Treatments
With no definitive guidelines about either the diagnosis or causes of FM, it only follows that opinions on treatment options are also varied and sometimes contradictory. Usually patients resort to a combination of medication and lifestyle changes to help relieve symptoms. The standard approach in the medical profession is to offer patients a range of specialists to treat individual symptoms: namely rheumatologists to advise on muscular and joint pain, neurologists for their knowledge of the central nervous system, and mental health specialists to offer support for depression.
Increasingly, illnesses such as FM and Chronic Fatigue Syndrome which are eluding the medical profession, are being successfully managed by alternative therapies. The London-based Optimum Health Clinic specializes in the treatment of illnesses such as FM as well as ME and Chronic Fatigue Syndrome.
The treatment of FM can be frustrating for both patients and their physicians and it is important for people with FM to become active participants in their own health care, not just recipients. But by learning self-management techniques, they will be able to handle their symptoms more effectively and hopefully return to a lifestyle virtually free of symptoms. Education is essential for this process: local support groups and charities can be extremely beneficial in gaining greater understanding of this often misdiagnosed and misunderstood condition, and there are some success stories out there to help you remain hopeful of a recovery.
Some useful links:
www.theoptimumhealthclinic.com
FibroFix.com and The Fibro Fix David Brady
Image Attribution:
"pain-map" (CC BY-NC-ND 2.0) by vaXzine
Subscribe Here!
Recent Posts
Meningococcal Infections: The Ongoing Need for Early Diagnosis in the UK (2026 Update)
Meningococcal infections (including meningococcal meningitis, meningococcal septicaemia, and..Isabel DDx Companion with ChatGPT Integration - to help you diagnose even faster
At Isabel Healthcare, we’ve always been driven by one goal: to make clinical reasoning faster,..List Of Categories
- Differential Diagnosis Decision Support
- Differential diagnosis
- Symptom Checker
- Symptoms
- Patient Disease Information
- Medical Error
- Disease
- Clinical Decision Support
- Diagnostic Decision Support
- Isabel 1 Minute Read
- Diagnosis Error
- Diagnosis Skills Cases
- Healthcare Informatics
- Clinical Reasoning
- Evidence-based Medicine
- Medical Education
- Patient Engagement
- Symptom Triage
- Nurse Practitioner Education
- Nursing Decision Support
- Partnership
- Public Health
- COVID-19
- EHR
- Patient Empowerment
- Patient Safety
- rare disease

Start your FREE Trial today
Try the Isabel Pro DDx generator for 30-days - no payment card details required.




