- Privacy Policy
- Terms & Conditions
- Contact us
- ©Isabel Healthcare 2025
1 Minute Read | Fibromyalgia | Isabel Healthcare
A research article in Journal of Anesthesia & Pain Medicine was published recently, detailing a review on patients referred with a diagnosis of fibromyalgia. The review found that the diagnostic criterion for fibromyalgia was not met in 97.3% of the patients referred, indicating that the condition is often over diagnosed. It was also found the referring physicians failed to diagnose 133 (94.3%) medical conditions in these patients which can be determined as an error of omission. The authors commented that ‘fibromyalgia may have become the “disease de jour” for the medical community and the absence of strict adherence to the diagnostic criteria for diagnosing fibromyalgia has led to many missed diagnoses.”
What is Fibromyalgia?
Fibromyalgia, also known as myofascial pain syndrome, fibrositis or fibromyositis, is a chronic, noninflammatory diffuse pain disorder which is represented by widespread musculoskeletal pain. It has a chronic disease course, although improvement in symptoms may occur in approximately 25% of untreated patients every 2-3 years. It predominantly affects females more than males where 70-90% of sufferers are females. The age range affected is normally those within 20 to 65 years of age. Prevalence has been reported as 1.1% of the adult US population and 8% of primary care patients. The cause of fibromyalgia is unknown but it is related to abnormal pain processing within the peripheral, central and sympathetic nervous system.
Symptoms and Diagnosis of Fibromyalgia
The primary complaint is chronic widespread pain for longer than 3 months. Other symptoms do vary but may include:
- fatigue
- sleep disturbance
- morning stiffness
- headaches which are tension and migraine types
- mood disorders including depression, anxiety and panic disorders
- sexual dysfunction
- regional pain syndromes including irritable bowel syndrome, chronic pelvic pain or vulvodynia
The key to diagnosing fibromyalgia is assessing if the following diagnostic criteria are found based on the American College of Rheumatology 2010 guidelines.
- widespread pain index above 7 and symptom severity scale score above 5
- symptoms present for longer than 3 months
- absence of any other disorder which would explain the pain
Therefore, it is important to work up a detailed history and a thorough physical examination of the patient, which includes a differential diagnosis where other causes for the pain are investigated and ruled out before a diagnosis of fibromyalgia can be made.
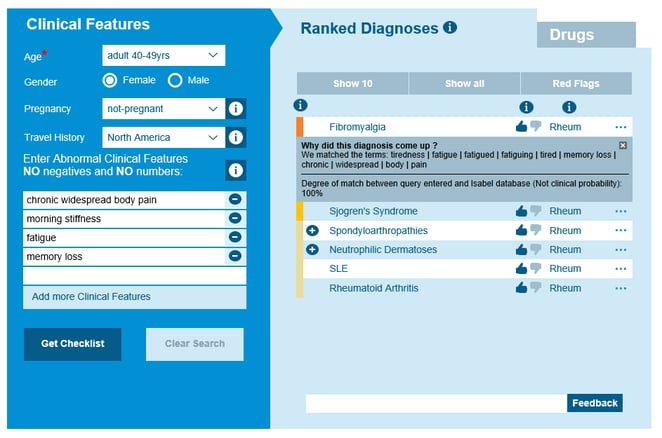
Isabel differential diagnosis for fibromyalgia type symptoms and what to consider
In order to rule out all other diseases being considered, lab testing is normally performed and these tests can include:
- complete blood count
- erythrocyte sedimentation rate (ESR)
- C-reactive protein (CRP)
- creatine kinase
- metabolic panel
- thyroid function test
- routine testing for ANA or rheumatoid factor is only carried out if you are considering the cause may be an autoimmune disorder or if initial ESR and/or CRP are abnormal
- screen for sleep apnea and repetitive limb movements with an overnight polysomnogram
Imaging is not indicated unless it is needed to exclude other diseases from the differential which may have presented.
Treatment of Fibromyalgia
Nonpharmacologic treatment is critical to successful outcomes. These management strategies include encouraging the patient to be an active participant in their care especially regarding exercise and a healthy lifestyle. Regular exercise and sleep management strategies have led to improved outcomes. Educating the patient about their diagnosis is key to them managing their condition. Complementary and alternative therapies including acupuncture and yoga may also help the patient manage their condition.
If pharmacologic intervention is needed it should be guided by symptoms and may require a combination of medications. Pharmacological treatment can include medications such as:
- antidepressants may improve pain, fatigue and depressed mood in patients diagnosed with fibromyalgia
- antiepileptic medications may be effective to modulate pain
- analgesics
- a trial of pharmacologic cannabinoid may be helpful in patients with fibromyalgia and sleep disturbance
Follow ups with frequent visits from the time of diagnosis and treatment commencing is extremely important. At first there may be more visits needed so symptom progression and resolution can be monitored with the treatment and lifestyle modifications which have been decided upon in the treatment plan. The support provided by professionals is important to manage the patient’s condition and achieve successful outcomes.
As the research article indicated, Fibromyalgia is a complex disease which is difficult to diagnose unless you have rigorously applied the diagnostic criteria for reaching a confirmed diagnosis. This includes ruling out other diseases which have the same symptoms as fibromyalgia on your differential diagnosis checklist. Isabel can help you work through these differential diagnoses until you have reached your final confirmed diagnosis of fibromyalgia which will enable you to avoid overlooked or missed diagnoses and your patient receives better patient care with a thorough differential diagnosis workup.

Mandy Tomlinson
Mandy has worked for Isabel Healthcare since 2000. Prior to this, she was a Senior Staff Nurse on the Pediatric Infectious disease ward and high dependency unit at one of London's top hospitals, St Mary’s in Paddington which is part of Imperial College Healthcare NHS Trust. Her experience in the healthcare industry for the past 33 years in both the UK and USA means she's a vital resource for our organization. Mandy currently lives and works in Scottsdale, Arizona.
Subscribe Here!
Recent Posts
Meningococcal Infections: The Ongoing Need for Early Diagnosis in the UK (2026 Update)
Meningococcal infections (including meningococcal meningitis, meningococcal septicaemia, and..Isabel DDx Companion with ChatGPT Integration - to help you diagnose even faster
At Isabel Healthcare, we’ve always been driven by one goal: to make clinical reasoning faster,..List Of Categories
- Differential Diagnosis Decision Support
- Differential diagnosis
- Symptom Checker
- Symptoms
- Patient Disease Information
- Medical Error
- Disease
- Clinical Decision Support
- Diagnostic Decision Support
- Isabel 1 Minute Read
- Diagnosis Error
- Diagnosis Skills Cases
- Healthcare Informatics
- Clinical Reasoning
- Evidence-based Medicine
- Medical Education
- Patient Engagement
- Symptom Triage
- Nurse Practitioner Education
- Nursing Decision Support
- Partnership
- Public Health
- COVID-19
- EHR
- Patient Empowerment
- Patient Safety
- rare disease

Start your FREE Trial today
Try the Isabel Pro DDx generator for 30-days - no payment card details required.




